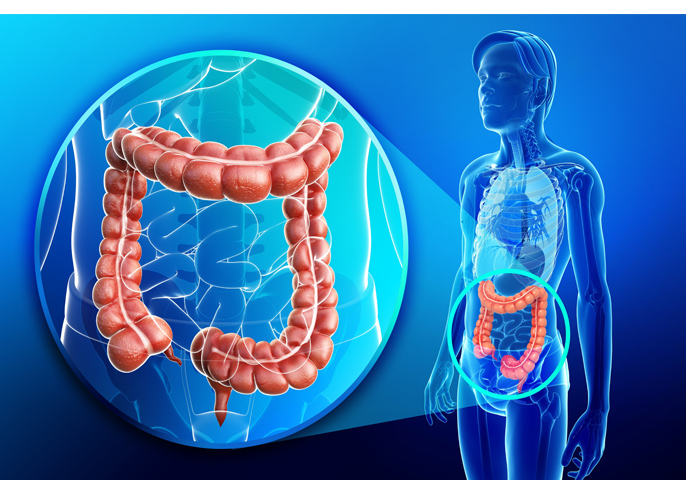

Colorectal cancer is a very insidious disease which can be present without any visible symptoms for a long time. Colorectal cancer develops as a result of uncontrolled cell growth within one of the parts of the large intestine (the caecum, the transverse colon, the ascending colon or the rectum). In most cases, the cancer develops from adenomatous polyps (adenomas), i.e. benign tumours of the epithelial tissue of the intestine which may over time transform to become malignant. Adenomatous polyps are in the form of small mucosal protrusions, develop without symptoms and occur on average in 20-40% of people who had a colonoscopy performed. The cancer is more frequent in men than women, and the highest number of incidents occurs after the age of 70 years. In Poland colorectal cancer is the second most common cause of death due to cancer.
FACTORS INCREASING THE RISK OF DEVELOPING COLORECTAL CANCER
The most common among the factors that increase the risk of developing colorectal cancer include:
- genetic predispositions – the risk of incidence is significantly higher in people with a family history of colorectal cancer
- presence of adenomas in the large intestine
- inflammatory bowel disease – chronic bowel inflammation, such as ulcerative colitis or Crohn’s disease, increase the risk of cancer
- incorrect diet based on large amounts of fats and red meat and poor in fibre is a risk factor
- smoking
- excessive use of alcohol
- a sitting lifestyle – lack of physical activity considerably increases the risk of colorectal cancer
- diabetes and insulin resistance
- age – a vast majority of people with the disease are over 50 years of age
- patients who were treated for colorectal cancer in the past


SYMPTOMS OF COLORECTAL CANCER
Colorectal cancer can develop in any section of the intestine but most cases, i.e. over 70%, develop in the rectum. Here is what should be worrying you:
- presence of blood in faeces after defection
- occult bleeding (i.e. positive result of the faecal occult blood test)
- rectal bleeding (recurrent)
- changes in bowel habits (alternating between diarrhoea and constipation)
- changes in the shape and size of stools, particularly so-called pencil-thin stools
- sensation of being unable to empty your bowels completely
- persistent diarrhoea
- chronic abdominal pains and cramps
- abdominal pain with retention of gases and stools indicating gastrointestinal obstruction
- nausea
- faecal urgency and inability to pass stools
- loss of body weight, anaemia, tiredness and lack of appetite – symptoms occurring in the advanced stage of the disease.
COLORECTAL CANCER DIAGNOSIS
There are many examinations that enable detection of colorectal cancers. It is the doctor’s responsibility to decide on the choice of method and the sequence of the individual examinations based on an interview with the patient. The most common methods used in diagnosing colorectal cancer are as follows:
- A ‘per rectum’ (rectal) examination – this is one of the basic diagnostic methods. The physician slips a lubricated finger into the rectum through the anus and palpates the lower part of the rectum. In this way they can feel and identify a large number of tumours located in this part of the large intestine.
- Proctoscopy – rectal endoscopy. In the examination a rigid optical instrument is inserted into the rectum. Proctoscopy enables visualisation of approx. 25 cm of the end section of the large intestine (rectum and sigmoid colon). If necessary, it is also possible to collect a sample of the suspected lesion. The examination is completely painless and is performed without anaesthesia.
- Colonoscopy – this examination is performed by means of a flexible endoscope. During the examination, a special endoscope with a camera that can transmit images to the outside fitted at the tip is introduced into the patient’s rectum. This method makes it possible to visualise the mucosa of the whole large intestine (as far as the ileocecal valve, which separates the small intestine and the large intestine). If necessary, it is also possible to collect a sample of the suspected lesion.
- Virtual colonoscopy – in the procedure air is pumped into the bowel and then abdominal CT is performed. The examination makes it possible to obtain a three-dimensional image of the large intestine and to visualise any lesions in the bowel.
- Barium enema – in this examination the colon is filled with a radiocontrast agent and air, and then a number of X-ray images are taken, which enables visualisation of any possible lesion in the bowel.
- Testing for the presence of occult blood in the stool – this is a minimally invasive test which detects presence of blood that is not visible to the naked eye in the stool.
- Testing for carcinoembryonic antigen (CEA) in the blood – this is a blood test in which markers characteristic for colorectal cancer are measured.

 +48 785 054 460
+48 785 054 460